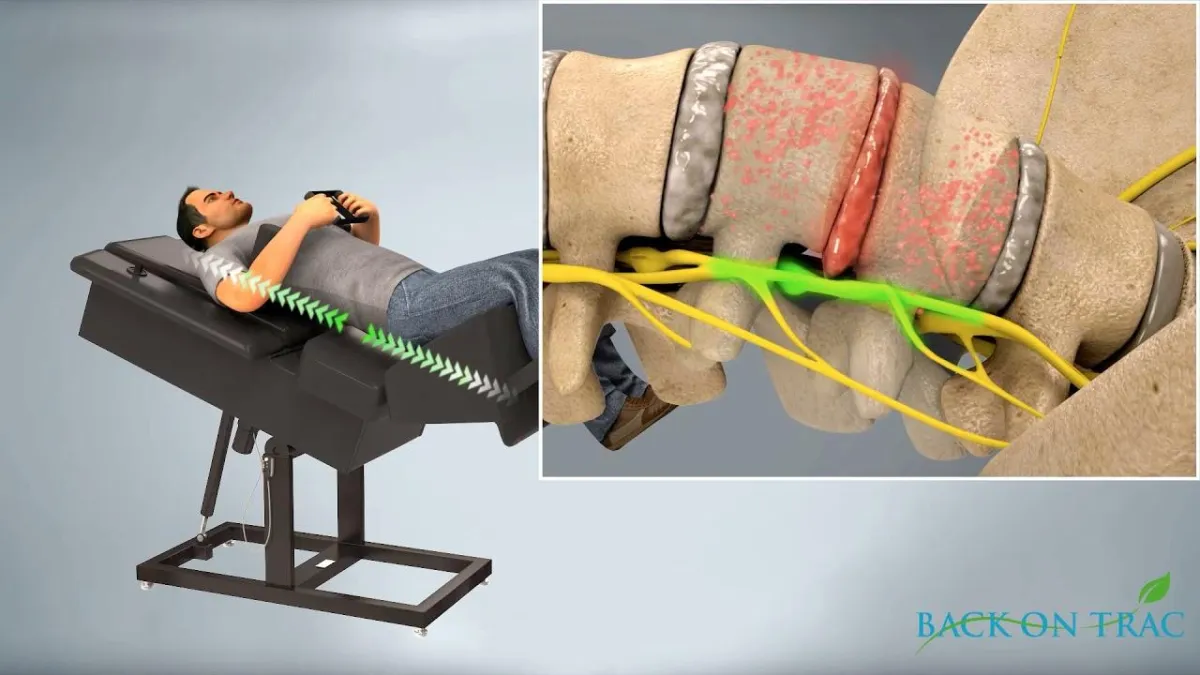
How Spinal Decompression Works: A Mechanical Explanation
When people suffer from chronic back pain, disc injuries, or sciatica, they are often told their options are limited to medications, injections, or surgery. While these approaches may be appropriate in certain situations, many patients want to understand whether there are conservative ways to address the mechanical causes of spinal pain.
One therapy that is often discussed in this context is non-surgical spinal decompression.
Spinal decompression therapy is designed to reduce pressure within the spinal discs and create more space around irritated nerves. By addressing the mechanical stress affecting the spine, this therapy may help some individuals experiencing disc-related back pain or sciatic nerve symptoms.
Understanding how spinal decompression works requires a closer look at the structure of the spine and the forces that affect spinal discs.
Understanding the Structure of the Spine
The human spine is composed of vertebrae, which are the bones stacked on top of each other that form the spinal column.
Between each vertebra sits a small cushion called an intervertebral disc.
These discs perform several critical functions:
• Absorbing shock during movement
• Allowing the spine to bend and twist
• Maintaining spacing between vertebrae
• Protecting nearby spinal nerves
Each disc contains two main components:
The outer ring (annulus fibrosus):
A tough outer layer made of fibrous tissue that holds the disc together.
The inner center (nucleus pulposus):
A soft gel-like core that helps distribute pressure evenly.
When discs are healthy and hydrated, they help maintain proper spinal alignment and nerve spacing.
However, over time discs can become damaged due to factors such as:
• Aging
• Repetitive spinal stress
• Poor posture
• Prolonged sitting
• Injury or trauma
These changes may lead to conditions such as disc bulges or herniations.
If you want to understand how these conditions differ, read:
Bulging Disc vs Herniated Disc: What’s Actually Causing Your Pain?
What Happens When Disc Pressure Increases
Many cases of back pain and sciatica develop when spinal discs experience excessive internal pressure.
This pressure may increase due to:
• Prolonged sitting
• Heavy lifting
• Poor posture
• Repetitive spinal strain
When pressure inside a disc increases, the disc may begin to bulge outward. In more severe cases, the outer wall of the disc may weaken enough to allow the inner material to push outward, creating a herniation.
These structural changes can reduce the space around nearby spinal nerves.
When nerve roots become irritated or compressed, symptoms may appear such as:
• Lower back pain
• Pain traveling down the leg
• Tingling or numbness
• Muscle weakness
• Sciatica
Why Sitting Can Increase Disc Pressure
One of the most common contributors to disc pressure is prolonged sitting.
Research has shown that sitting increases pressure inside spinal discs more than standing or walking.
When someone sits for extended periods:
• The pelvis tilts backward
• The natural curve of the lower spine flattens
• Disc pressure increases
• Core muscles become less active
Over time, this increased pressure may contribute to disc degeneration and nerve irritation.
If sitting worsens your back pain, you may find this helpful:
Why Sitting Is Quietly Destroying Your Spinal Discs
What Spinal Decompression Is Designed to Do
Spinal decompression therapy is designed to reduce pressure inside the spinal discs.
This therapy uses a specialized computer-controlled table that gently stretches the spine using precise traction forces.
The goal is to create a temporary reduction in disc pressure.
This reduction in pressure may help:
• Reduce stress on damaged discs
• Increase space around compressed nerves
• Encourage fluid movement within the disc
• Support the spine’s natural healing processes
This mechanical approach is different from treatments that focus primarily on reducing inflammation.
How Decompression Creates Negative Disc Pressure
One of the key concepts behind spinal decompression therapy is the creation of negative disc pressure.
Negative pressure occurs when the traction forces applied to the spine gently separate the vertebrae.
This separation may allow the disc to temporarily create a small vacuum-like effect inside the disc.
In some cases, this process may help:
• Draw fluid back into the disc
• Reduce pressure on disc structures
• Decrease stress on nearby nerves
This process may also improve the exchange of nutrients within the disc.
Healthy discs rely on fluid movement to maintain hydration and structural integrity.
How a Decompression Table Works
Modern spinal decompression systems use computer-controlled traction to ensure precise and safe treatment.
During therapy:
• The patient lies comfortably on a decompression table
• A harness is placed around the hips or torso
• The table applies gentle traction cycles that slowly stretch and relax the spine
These traction cycles are carefully controlled to prevent the body from triggering protective muscle spasms.
This controlled approach allows the spine to gradually experience decompression forces.
Why Controlled Traction Matters
Traditional traction methods have been used for decades, but older traction systems sometimes caused muscles to tighten in response to the pulling force.
Modern spinal decompression systems are designed to apply traction in specific patterns that help minimize muscle resistance.
These controlled cycles allow the spine to experience gradual decompression while remaining comfortable.
This approach helps target the spinal discs rather than simply stretching surrounding muscles.
What Conditions May Benefit From Decompression
Spinal decompression therapy is often considered for individuals experiencing disc-related spinal conditions.
These may include:
• Bulging discs
• Herniated discs
• Degenerative disc disease
• Sciatica
• Chronic lower back pain
However, decompression therapy is not appropriate for every spinal condition.
A proper evaluation is necessary to determine whether the therapy may be suitable.
Why Imaging Results Don’t Always Match Symptoms
Some individuals experience severe symptoms despite imaging that shows only minor structural changes.
Others may have visible disc abnormalities but minimal pain.
This occurs because MRI scans show the structure of the spine but cannot always capture how the spine behaves during movement.
To better understand this concept, read:
Why Your MRI Says “Normal” But You Still Have Back Pain
Why Some Treatments Focus Only on Symptoms
Many common treatments for back pain aim to reduce inflammation.
These treatments may include:
• Anti-inflammatory medications
• Physical therapy
• Steroid injections
While these approaches can provide relief, they may not always address the mechanical pressure affecting spinal discs.
When Surgery May Be Necessary
Although many disc-related conditions can be managed conservatively, surgery may sometimes be required.
Situations where surgery may be recommended include:
• Progressive nerve damage
• Severe spinal instability
• Loss of bowel or bladder control
• Advanced disc herniation
Understanding when surgery is appropriate can help patients explore treatment options more confidently.
Understanding the Different Types of Sciatica
Sciatic nerve pain can originate from several different spinal conditions.
Common causes include:
• Disc compression
• Spinal stenosis
• Piriformis muscle irritation
• Degenerative spinal changes
Because the underlying cause varies, treatment approaches should be tailored accordingly.
Learn more in:
The 3 Types of Sciatica (And Why Treatment Must Match the Cause)
Learn More About Spinal Decompression
If disc pressure or nerve irritation may be contributing to your back pain or sciatica, understanding your treatment options is an important step.
Explore our complete guide to Non-Surgical Spinal Decompression for Chronic Back Pain and Sciatica to learn more about how this therapy works and whether it may be appropriate for your condition.
